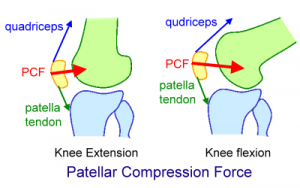
The patella is a site of incredible load transmission, and it is frequently a pain generator in people doing a lot of running and jumping.
Patellofemoral pain syndrome is an umbrella term for a large number of disorders that cause pain at the front of the knee joint.Patellofemoral pain syndrome is an umbrella term for benign conditions that cause pain over the front part of the knee surrounding the patella. Specific diagnoses which would fall under this umbrella would include patellar tendinopathy, Osgood-Schlatter‘s disease, chondromalacia of the patella, patellar maltracking syndromes, patellar subluxation, quadriceps tendinopathy and patellar plica syndrome. Patellofemoral pain is common in virtually all patients from young to old. It is particularly common in young people doing lots of running and jumping. I like to think of patellofemoral pain syndrome as an “ailment”, and the acronym AIL helps to organize my thoughts in the assessment of this condition.
[/x_blockquote]
Think of patellofemoral pain as an “AILment”, characterized by Alignment problems, Imbalance of musculature and Loading.
The “A” stands for alignment issues, asindividuals who have patellofemoral pain often have relatively flat, pronated feet associated with genu valgum or knocked kneed posture. This is often associated with an internally rotated hip and the presence of hip abductor muscle weakness.
The “I” stands for imbalance of musculature as people often have relatively weak quadriceps in relationship to their hamstrings. As mentioned, relative weakness of the hip abductors is particularly problematic in the genesis of patellofemoral pain. Weak quadriceps, shortened hamstrings and shortened lateral hip structures are also thought to contribute.
The “L” stands for loading and most people with patellofemoral pain syndrome have been exposing their legs to significant loading, particularly running, jumping and stop/start change direction activities.
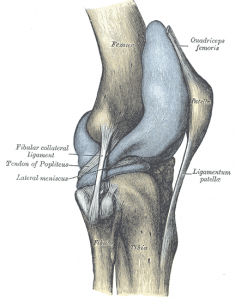
In general, people with patellofemoral pain do not have significant locking, swelling or giving way of the knee. The presentation is usually insidious with no inciting traumatic event. Most people have been increasing their load in the weeks to months before the onset of patellofemoral pain problems.
Physical examination is done to rule out other knee joint conditions. Usually, there are normal ligaments, no fluid in the knee joint and full range of motion on assessment. The inferior pole of the patella and the medial patellar facets are often tender to palpation and can reproduce the patient’s pain experience. Important things to look for on assessment include the presence of dynamic valgus and weakness of the hip abductors, as these are two of the most common culprits in the genesis of this syndrome.
X-rays will sometimes be done to rule out loose bodies or the presence of other joint disease such as arthritis. Generally, these are normal. Useful information can be gleaned from the use of patellar x-rays. These patellar x-rays sometimes called skyline views demonstrate the position and station of the patella in relationship to the groove that it is suppose to track in, on the femur. Typical examples of anatomic changes that contribute to patellofemoral pain include significant lateral tracking of the patella. It is thought that muscle imbalance with weakened medial anchors including the vastus medialis and shortened lateral traction muscles including the iliotibial band are responsible for this so-called patellar maltracking.
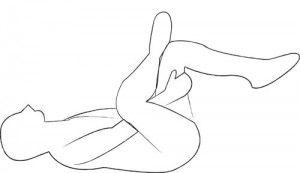
In general, all aspects of the ailment need to be treated for patellofemoral pain problems. Flat footedness and dynamic valgus needs to be dealt with by either footwear, orthotics or specific muscle strengthening exercises. Muscle imbalances need to be addressed with weak muscles being strengthened and shortened muscles being lengthened. The figure four stretch helps to relax the shortened lateral attachments to the patella that emanate from the iliotibial band.
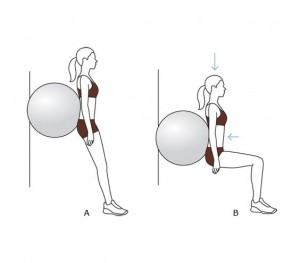
The wall squat is a safe and effective way of strengthening your quadriceps, gluteals and hamstrings. Squeezing a ball between your knees doing a wall squat is a good way of activating your inner thigh muscles at the same time. Try not to go too deep in the wall squat, as the pressure behind the knee cap increases in proportion to the depth of your squat. In very angry knees, I have patients stop the squat at 45 degrees.
Sometimes patellar stabilizing sleeves are used to decrease pain and help to optimize patellar tracking. These are widely available. The application of some topical pain controlling/anti-inflammatory medicines sometimes help with the pain experience but taking medications by mouth is usually not required.
Most patients with patellofemoral pain problems report that their pain is worse after activities than it is during activities. The classic manifestation of this is the theatre sign where individuals have pain sitting in a confined space such as driving home from a game or in a movie theatre.
In general, this condition can be successfully treated with the interventions described here.
