
Having practiced medicine for over 30 years, I have noticed numerous significant developments. When I was in medical school, the human immunodeficiency virus and the entire AIDS syndrome was really an unknown entity. Also, a very interesting area of technology, Magnetic Resonance Imaging or MRI was in its infancy. This type of imaging was applied to the evaluation of musculoskeletal problems and provided amazing insight into the anatomy of the musculoskeletal system. This was considered to be a substantial boon in the evaluation of many musculoskeletal problems. The use of MRI was rapidly applied to problems such as back pain and areas of disc degeneration and disc dessication were identified with greater clarity than ever before. In certain regions of the United States, surgeons began operating on these degenerative discs. Unfortunately, a generation of so-called failed back syndromes followed as people did not improve as anticipated after their back surgery. A seminal publication in the early 1990’s was entitled “MRI, Terrific Test or Tar Baby”. It highlighted the fact that some of the anatomic features identified on MRI were actually normal age-related changes and frequently found in people with no back pain. They were not indications for surgery. I find this lesson is one of the hardest to learn in the assessment of patients with musculoskeletal problems. I also find that patients seem to have a disproportionate amount of faith in MRI technology and view it as a truth serum. Earlier in my career, I tried to convince patients not to have MRI’s as I thought my clinical examination was more important to them. I’m not sure I succeeded in winning many of those arguments.
The MRI is a very valuable tool at ruling out sinister problems in the musculoskeletal system. It is a very sensitive modality to rule out tumors, infections or subtle fractures that are not obvious on plain x-ray. This is especially true in the assessment of spinal pain patients. After this incredibly useful component of MRI technology, it frequently reveals age-related degenerative changes. These age-related degenerative changes are present in many people who have no symptoms despite the degeneration in that particular body part. For example, 60% of 60-year old men have tears in their rotator cuff on MRI despite having no symptoms in their shoulder. 50% of men who are 50 have horizontal cleavage tears of their medial meniscus in both knees but have no symptoms. The majority of people over the age of 40 will have degenerative changes in their cervical and lumbar spines but have no symptoms.
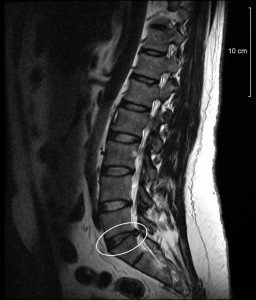
This MRI shows a disc abnormality. This may or may not lead to pain.
This indicates that we can have degeneration of important structures without clinical findings or pain. Therefore, we need to be quite discerning when attributing pain to the findings we see on an MRI.
This poses an interesting problem to the clinician when you visit them complaining of pain in your shoulder, knee or back, without a significant episode of preceding trauma. If your shoulder simply gets sore when you’ve been doing some raking or some overhead work, and an MRI is done revealing a rotator cuff tear, did the patient tear the rotator cuff with their simple housecleaning activities? The answer is probably not. This takes us back to the notion of the perturbation: we perturb an area of degenerative change in the musculoskeletal system and this is associated with pain. The area of the perturbation will often improve with appropriate care, but the area of degeneration does not heal. I frequently tell patients that the MRI will reveal the areas of our body that are drying, rotting and degenerating, but may not reveal the area of our bodies that is responsible for our pain syndrome.
In general, abnormal findings on MRI do not justify surgical procedures, as many patients can have degeneration of those areas and full function. MRI’s are still done to rule out sinister problems and these are often driven by specific patient complaints known as red flags. In the context of red flags, MRI’s are an important part of the medical assessment. Given the fact that they have no radiation, an MRI is usually safe for the patient. Clinical evaluation will often indicate other things are the pain generator besides the area of abnormality revealed by the MRI. Also, clinical evaluation can reveal the nature of a problem in a high degree of sensitivity and specificity without the extra expense needed through the use of an MRI. A simple example would be an anterior cruciate ligament tear of the knee where an experienced clinician can demonstrate the absence or presence of a normal ACL close to 100% of the time through two or three clinical tests known as the Lachman test, the drawer test and the pivot shift test. The Lachman test in particular has an exceptionally high level of sensitivity and specificity.
I would hope that my patients would be less interested in getting an MRI and more interested in getting a thorough and comprehensive clinical assessment. I think the MRI can be a terrific test, but it can also be a tar baby where it gives us information that we find actually clouds the assessment, and causes the patients a great deal of unnecessary worry.
Magnetic resonance imaging of the lumbar spine. Terrific test or tar baby?
